
Healing Spaces: Healthcare Design Past, Present and Future

Hospital (Noun):
An institution that is built, staffed and equipped for the diagnosis of disease; for the treatment of the sick and injured; and for their housing during this process. Modern hospitals often serve as a centre for investigation and for teaching. (Britannica)
Etymology:
hospes (Latin) – meaning stranger or foreigner. Came to mean ‘guest’. Hospitum (Latin) – the relationship between a guest and shelterer; hospitality; friendliness and hospitable reception.
Throughout known human history, healthcare spaces have always been in existence. These spaces have appeared in many forms depending on factors such as time, location and cultural beliefs. The common factor though has often been physical buildings created for the purpose of healing.
Healthcare spaces are not limited, and never have been limited, to hospitals but a hospital is generally the key space that we associate with healthcare. From care within the home and community to end of life care in a hospice, and from urban to rural areas, we all access healthcare in different ways in different times of need.
Florence Nightingale used her nursing experiences in hospitals, as well as prolonged periods of her own ill health, to make informed choices about the design of the spaces she worked in from both a nurse and a patient perspective. Her expertise was respected, and she became and advisor to architects and hospital boards across the world.
In this exhibition we have partnered with experts in the field today to display a range of case studies highlighting key healing spaces from ancient times through to the work being done today for our spaces of the future.
Healthcare Design Today
We have worked with some wonderful partners for this exhibition, hearing stories from across the glode demonstrating the work being done on healthcare design today and for the future.
Do you have a case study or story on healthcare design & nurses that you would like to contribute to this online exhibition? Please get in touch! Please use subject title ‘Healing Spaces Case Study’.
Please note that we will be reviewing case studies before publishing on the online exhibition. Unfortunately, we will not be able to publish all case studies but would still love to hear from you.
American College of Healthcare Architects
Nursing Institute of Healthcare Design
NHS New Hospital Programme
Debbie Gregory
HGA
Belmont University
Montana State University
HKS
Yellow Brick Consulting, Inc.
HCA
Queens Institute of Community Nursing
Taichung Tzu Chi Nursing Home
Mbarara University of Science and Technology
Trinity Western University
Changhua Christian Hospital
Károlyné Boros

American College of Healthcare Architects
The American College of Healthcare Architects [ACHA] provides Board Certification for Architects who practise as healthcare design specialists. Our mission is to distinguish healthcare architects through certification, experience and rigorous standards. Our vision is transforming healthcare through better built environments.
The ACHA was founded in 2000 and is celebrating its 25th anniversary in 2025. ACHA Certification for the practice of healthcare architecture is the only speciality recognised by the American Institute of Architects and is also endorsed by the American Society of Healthcare Engineers [ASHE].
ACHA certificate holders include architects throughout the United States and Canada with specialised skills and proven expertise. As of 2025, there are 504 licensed and actively practising architects that are board certified by the College. An additional 104 certificate holders hold emeritus status in the College.
To receive ACHA Board Certification, healthcare architects must document their experience and demonstrate their skills through a computer-based examination, references and a portfolio review of their work experience. Licensed Architects from the UK, Australia and other countries recognised for reciprocal licensure in the US by the National Council of Architectural Registration Boards [NCARB] are also eligible to apply for ACHA Certification.
ACHA Certificate holders work toward improving the evidence-based design of healthcare architecture on behalf of the public, practise in an ethical manner, maintain high standards of specialised continuing education and add to the body of knowledge. Our certificate holders are recognised as pioneers and industry leaders in the design of healthcare facilities throughout the US and around the world. They routinely develop, present and share knowledge on evidence-based best practice for healthcare facility design in national and international forums.
Further information on the American College of Healthcare Architects can be found on our website at: https://healtharchitects.org/about/.

Nursing Institute for Healthcare Design, USA
In 2005 Debbie Gregory, a registered nurse, returned to school to study interior design and pursue a love for space planning and design.
While studying programming, schematic design and then researching and designing for healthcare projects, the chasm of understanding between the two fields became particularly apparent to her. She wondered, “Is anyone asking the nurses about their opinions on the design and function of their work environments?” and began investigating.
To her surprise, there was little data from the nursing community. The only research she found was in the emerging field of evidence-based design. She felt strongly that nurses could be contributing significantly to research and design decisions, so contacted her colleague, Laura Hayes. They began researching healthcare design and determining how nurses can contribute as part of the design team. At a Healthcare Design Conference in 2005, they managed to set up an impromptu meeting for nurses in the audience. Ten nurses attended and the database of nurses in healthcare design was born.
The conference began the path to determine where the nurse fits into the design process and what role the nurse should contribute as a part of the design team. Debbie realised that a nurse could be the interpreter between the two professions, both literally to translate professional terms and to bridge the culture and communication gaps. More importantly, Debbie realised she could help designers pose the right questions, which were all critical to achieving successful facilities.
Laura and Debbie officially launched the Nursing Institute for Healthcare Design (NIHD) in 2010. As a not-for-profit association, it is dedicated to educating and inspiring nurse leaders about their role in healthcare design and construction. The organisation provides tools and research, peer education and mentoring and a connection to other members.
On the design side, architects, contractors, facility managers, hospital administrators and clinicians have become involved and want to impact this new collaborative relationship that will facilitate trust, respect, shared goals, improved clinical work environments and ultimately patient outcomes. Many in the design community are now investing to place clinicians on their staff to educate and facilitate between their staff and their clients. This has given nurses a voice and an advocate. Hopefully, this is just the beginning of a future design collaborative that is patient and end-user centred.

The New Hospital programme is a National Health Service (NHS) and UK Governement scheme for the future of building hospitals in England. It is working to transform the way that hospitals are designed and built, providing world-class innovations and infrastructure for the healthcare sector. The New Hospital Programme (NHP) is replacing outdated hospital facilities with modern and environmentally sustainable buildings to provide exceptional healthcare services and facilities for patients, staff and local communities. Digital technology is changing the way healthcare is delivered in these facilities and the use of smart technology will reduce basic and repetitive tasks, freeing up time for patient care.
Clinicians and staff from all areas of the healthcare sector, including doctors, nurses, architects and professionals from a wide range of industries, have been closely involvoed in the designs of the New Hospital Programme, bringing lifetimes of experience and knowledge on best practices.
Hospital 2.0 is the name for a series of designs that hospitals will use in the future. Rather than treating each hopsital as a stand alone design, NHP is standarising designs across projects, ensuring that all future hospitals have the same facilities for patients and staff across the country. The nature of Hospital 2.0 is that designs are iterative, meaning that they will be continuously updated with newest advances in methodologies to ensure best health outcomes for years to come.
Hospital 2.0 is a bit like lego, all the pieces are the same, but individual hospital trusts get to decide how many pieces they need and how they are put together to best serve the needs of the communities. This means that, for example, a hospital bedroom in Airedale will be identical to one in Cornwall. As a result, hospitals can be built much faster and more efficiently than in the past because hospital trusts don’t have to spend time and money creating their own designs for each project.
NHP hospitals will all be unique to the communities where they are built and NHP provides designs for individual components, like bedrooms, operating theatres and staff spaces. The hospital trusts decide what the make-up of the hospital needs to look like to best serve their local population.
One of the key features is NHP’s move to 100% single bedrooms. Using the Hospital 2.0 deisign offers a smarter, more cost effective way to build hospitals. Comapred to a hospital with a mix of single bedrooms and multi-bed wards, this approach reduces building size, cuts capital and running costs and improves patients patient care. Single rooms help lower infection rates, support faster recovery and offer greater privacy and dignity for patients.
In the past single rooms haven’t always been supported by smart technology needed to help staff deliver safe, efficient care. Hospital 2.0 changes that – combining physical design, with digital capability to create safer, more flexible environments for patients and staff alike.
Hospital 2.0 single bedrooms can be used for any patient, removing the need for seperate areas and speeding up admissions and discharges. They help control infection, reduce backlogs and increase operational flexibility. Overall, this approach delivers long-term savings and better care.
Other key features in the New Hospital Programme include digital wayfinding capabilities, on-call accommodation for staff, mandatory staff welfare space allocation and staff calm rooms.
Future examples of hospitals that will feature all aspects of the Hospital 2.0 design include Milton Keynes Hospital, Hillingdon Hospital and many more.
Key influences for the programme include principles of infection prevention and control methodologies which were largely developed by Florence Nightingale in the Crimean War. Inspiration was also drawn from the modular methods of construction which helped to implement hospital facilities in the Crimean War, like Brunel’s prefabricated hospital buildings at Renkioi.
Debbie Gregory DNP, RN, FAAN

Dr. Debbie Gregory is a nationally recognized nurse leader, designer and healthcare innovator whose career bridges the worlds of clinical practice, technology and the built environment. As Principal of Healthcare Innovation Consulting at Smith Seckman Reid (SSR), she leads multidisciplinary teams that help hospitals and health systems reimagine care delivery through intentional design—aligning people, place, process, and technology to improve outcomes for patients, providers and organisations.
A nurse for over 40 years, Dr. Gregory began her career at the VA Hospital in Nashville, Tennessee. Her early experiences on the frontlines of care inspired a lifelong commitment to designing better healthcare environments. After earning a degree in Interior Design from Watkins College of Art and Design, she discovered a disconnect between clinical needs and design decisions—a realisation that led her to co-found the Nursing Institute for Healthcare Design (NIHD) in 2005. Through NIHD, she created a national platform to elevate the nurse’s voice in facility planning and design, advocating for evidence-based environments that promote safety, efficiency, and wellness.
Dr. Gregory earned her Doctor of Nursing Practice in Health Innovation and Leadership from the University of Minnesota, where she developed her framework for healthcare innovation grounded in systems thinking and human-centred design. Her work as a consultant, educator and author has influenced projects at organisations where she has guided the integration of smart hospital technologies, virtual care and digital patient engagement tools.
A Fellow of the American Academy of Nursing, Dr. Gregory serves as Co-Editor of the Health Environments Research & Design (HERD) Journal and as Senior Fellow for Nursing Innovation at Belmont University. She is a frequent keynote speaker and international lecturer, known for translating complex design and technology concepts into clinical relevance. Her scholarship explores topics such as nurse well-being, virtual nursing and the convergence of digital and physical environments.
A visionary connector and mentor, she continues to empower nurses to claim their seat at the innovation table and lead the transformation of care delivery for generations to come.

Terri Zborowsky, Ph.D., RN, EDAC, CPXP
Senior Design Researcher, HGA, USA
Terri’s first career as a nurse has driven her passion as a designer and design researcher. She decided to follow in the footsteps of Florence Nightingale who understood that qualities of space, such as daylight, cleanliness and even the variety of spaces, impacted the stress of her patients. After years of working as a bedside nurse, Terri has spent the last 20 years actively engaging in practice-based research with architectural firms to advance the body of design research, to elevate the design process with evidence and empathy and to enlighten designers, and those who make design decisions, from a return-on-investment perspective.
Terri has always been inspired by Florence Nightingale’s methods as a design researcher to focus her own research on discovering how aspects of the built environment impact people. She has specifically looked at the impact on nurses and staff, as well as the most vulnerable patients and their families, including those with chronic medical issues, mental and behavioural health conditions and Neonatal Intensive Care Unit babies. Amplifying their voices and seeing their needs reflected in the design of spaces for their care is her greatest pleasure.
Terri’s impact in the design of healthcare spaces includes over 70 healthcare design projects, 65 presentations and 30 publications. Her 2010 co-authored study on nursing stations in the peer-reviewed Health Environments Research & Design (HERD) journal was pioneering, influencing over 250 authors in at least fifty publications. Her 2014 HERD article on Florence Nightingale’s Environmental Theory remains one of the journal’s most read articles.
Terri is committed to research, education and advocacy, empowering healthcare leaders and designers to embrace change using evidence, knowledge, and empathy. As one healthcare organisation shared, “Her unwavering patience, enthusiasm, and commitment to helping owners understand how we have a role and obligation to look beyond our project and see that we can, indeed, broadly impact the advancement of healthcare design, is unparalleled.”


Shaping Healing Spaces Together
Belmont University, Nashville, Tennessee, USA
Shaping Healing Spaces Together is a short documentary that captures an innovative, human-centred experiment in higher education, where the fields of architecture and nursing converge to design spaces that heal. The film reveals how the next generation of professionals is being trained not only to enter the workforce, but to transform it.
At the core of the story is a cross-disciplinary partnership between students, faculty and industry professionals who share a vision: that the design of space and the practice of care are deeply intertwined. The collaboration between architecture and nursing students aims to reimagine environments of healing and challenges them to think differently, listen deeply and find creative solutions to some of the most pressing global challenges in healthcare and the built environment.
The documentary follows this journey of learning, empathy and innovation, weaving together intimate classroom moments, design process footage and personal reflections. Faculty mentors guide students through a process that values curiosity as much as technical skill and compassion as much as creativity. Industry partners bring real-world perspective, showing how collaborative approaches can lead to more inclusive, sustainable and humane outcomes in healthcare design.
Ultimately, the film reminds us that healing is not limited to hospitals or clinics; it is a social and spatial endeavour that begins with collaboration, which then becomes an act of healing for the students who learn, the communities they serve and the world they are preparing to shape.
Belmont University is renowned for its flourishing culture of collaboration, innovation and community. This project embodies Belmont’s mission to prepare students not just for careers, but for lives of purpose.

Design in Rural and Frontier Contexts
Dr Elizabeth Johnson, Ph.D., MS-CRM, RN – Montana State University, Mark & Robyn Jones College of Nursing, USA
The faculty of the Mark & Robyn Jones College of Nursing conduct community-based research and teach students to address complex challenges in health care access, delivery and design. Located in Bozeman, Montana, USA, MSU is home to the state’s only College of Nursing offering undergraduate, master’s and doctoral-level education. With five campuses located across the state, the College is uniquely positioned to investigate the intersections of geography, equity and care infrastructure.
The College prioritises cross-sector collaboration and engagement with rural health systems, tribal health partners, design professionals and informatics specialists. In this supportive infrastructure, faculty members such as Dr. Elizabeth Johnson, Ph.D., MS-CRM, RN, lead studies focused on biobehavioural responses to health care environments in rural settings, virtual lighting and window systems to simulate natural elements in remote facilities and integrative technologies for information sharing across fragmented systems of care. These innovative projects examine how built and digital environments can be designed to reduce stress, improve safety and support culturally meaningful care in low resource environments.
Dr. Johnson also investigates how health care systems can be designed with, rather than simply for, the communities they serve. Her research emphasises participatory approaches to system redesign, particularly in Indigenous and frontier communities where health systems must often function across geographic, cultural, and jurisdictional boundaries. In these contexts, she studies how architecture, workflow and technology can be aligned to support both clinical effectiveness and community trust. Dr. Johnson and her team have developed an initiative called ‘The Kind Room’, which includes children as young as five in the design of adaptive, inclusive hospital rooms for paediatric, adolescent and young adult care.
Dr. Johnson’s contributions offer a systems-based approach to health care design where research, community engagement and education come together to inform environments that are not only efficient but celebrate the human spirit of healing others and self. The work is supported by interdisciplinary collaboration, locally grounded inquiry and can extend the reach and meaningfulness of care across diverse settings.


Transforming Healthcare Design: The Vital Role of Nurse Designers
HKS was one of the first architectural firms to recognise the value a nurse’s perspective can bring to healthcare facility design. Known as nurse designers, these professionals play integral roles as advisors, strategists and space planners, offering insights that significantly enhance the design and functionality of healthcare environments.
Nurse designers rely on their frontline experience to translate the language of care into design, ensuring that every space supports both patients and caregivers. With a holistic perspective, nurse designers collaborate with architects, planners and healthcare leaders to shape the future of care through strategy, visioning, and simulations. Their curiosity and willingness to experiment drive innovative solutions, resulting in spaces that function seamlessly, enhance safety and elevate the human experience of healthcare.
Jennie Evans was the first registered nurse to partner with healthcare architects at HKS, pioneering the integration of clinical insight into the design process. Jennie served as past President of the Nursing Institute for Healthcare Design and was a recipient of the Healthcare Design HCD10 Award for her executive leadership in advancing healthcare design through interdisciplinary collaboration.
Working as a member of the architectural team, Jennie helped to implement lean methodologies at Akron Children’s Hospital in Akron, Ohio when planning a 34,000-square-metre expansion facility. Entire hospital floors including inpatient units, surgical theatres and emergency department bays were mocked up using large cardboard divider walls. The team of designers and clinical leaders used lean simulation techniques to test the desired future state workflow and adjust the design before the building was constructed.
Nurse designers will stay at the forefront of health facility design as the healthcare environment moves toward the increased use of new technologies like AI, robotics and simulations.


Kelly Guzman, MN, RN, FAAN, EDAC
President and Founder of Yellow Brick Consulting, Inc.
Kelly Guzman is the dynamic founder of Yellow Brick Consulting, Inc., boasting over 35 years of experience in clinical care, healthcare administration and consulting. A former president of the Nursing Institute of Healthcare Design and a seasoned nurse, Kelly has built a reputation for visionary nursing leadership, strategic project management and collaborative team building.
Her career is marked by a passion for developing efficient, creative approaches to complex healthcare initiatives and her ability to lead teams through high-stakes projects with clarity and precision.
Under Kelly’s leadership, Yellow Brick Consulting has successfully become the premier name in healthcare transition and activation. Her team has completed more than 140 healthcare projects across North America. These projects span a wide range of specialties and operational challenges, consistently delivering results that exceed expectations. Kelly and her team have also contributed to the industry’s body of knowledge through two widely respected publications: “Simplifying the Complex: A Guide to Transition and Activation Planning for Healthcare Construction Projects” and “A Guide to Healthcare Facility Dress Rehearsal Simulation Planning”. These books offer practical insights and best practices drawn directly from real-world experience.
Yellow Brick Consulting is a specialised healthcare consulting firm focused on operations planning, project management, behavioural health, licensing and regulatory preparedness and activation planning. The firm’s mission is to deliver unparalleled project management expertise to the healthcare industry, ensuring every client experiences a seamless and successful day one. This mission is realised through a collaborative partnership model that places client goals and outcomes at the centre of every engagement.
The Yellow Brick team methodology integrates nursing best practices, Lean Six Sigma principles, evidence-based change management and proven project management techniques. This comprehensive approach provides clients with a simplified, actionable roadmap to success, tailored to the unique demands of each healthcare environment.


The Human Body and a Hospital
What comes to mind when you think of a hospital?
You’re probably imagining a bustling place filled with doctors, nurses, patients and beeping machines – a living, breathing system, much like the human body – where every cell, tissue and organ plays a unique role.
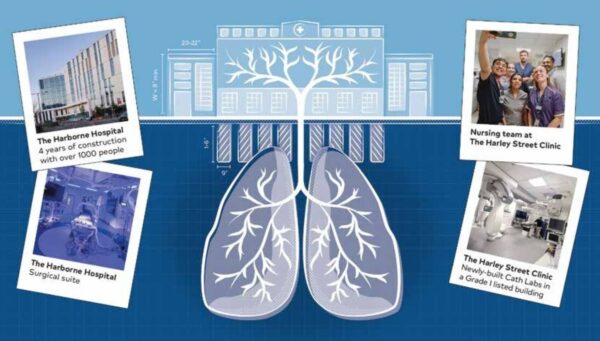
Take the respiratory system – it takes in oxygen and expels carbon dioxide. In a hospital this role is mirrored by air handling units (AHUs). Drawing in outside air, filtering dust, adjusting temperatures and distributing clean air throughout the building. AHUs, like our lungs, are vital to maintain a safe, healthy environment.
Water is also essential. Just as the human body comprises around 60% water, hospitals rely on robust systems for sterilisation, heating and cooling to provide exemplary patient care. New technologies now allow real-time tracking of water hygiene, much like heart monitors track vital signs to show how your body is functioning.
Then there is the skin, the body’s largest organ. Just like the hospital “skin” with its walls, floors and roofs, there are also the doctors, nurses, caterers, housekeeping and clerical staff, each of whom play a critical role in supporting and holding the hospital together.
Close collaborations between our clinicians, engineers, architects and infection prevention experts have created inspiring spaces that support safe, efficient and compassionate healthcare for all.
While the human body will not last forever, a well-designed, well-built and well-maintained hospital can serve and protect future generations to come.
At HCA UK, we actively incorporate the patient voice to shape environments that truly meet their needs, from brand new builds such as The Harborne Hospital, to our historical and heritage buildings of Harley Street. Through thoughtful design and teamwork, we ensure that heritage and innovation go hand in hand.

The Queen’s Institute of Community Nursing and the National Garden Scheme
Elsie Wagg Innovation Scholarship Programme for Community Nurses
The gardens and health movement promotes healthier lifestyles, self-care and reduced health inequalities. Gardens offer significant physical, mental and emotional health benefits. They help build confidence, encourage social bonds in safe environments and improve mobility and balance through physical activity. Simply being outdoors fosters a sensory connection to nature which can be transformative. Settings for nursing care, such as nursing homes and community health facilities, can revitalise gardens to reignite hobbies and improve wellbeing.
Garden to Plate Project
Led by Kendra Schneller, Queen’s Nurse, London
The aim of this project was to enhance mental health and wellbeing in homelessness services in Lambeth through therapeutic gardening and communal food activities.
This nurse-led initiative created a safe, inclusive space for growing, cooking, and sharing food. The garden itself was a previously neglected and unused space adjacent to community healthcare facilities. The project supported individuals facing mental health challenges and fostered informal engagement with healthcare services through trust and relationship-building.
Gardening and cooking together promoted resilience, confidence, and emotional stability. Participants reported reduced anxiety and increased motivation.
The key outcomes for the project were improved mental wellbeing and routine, a greater awareness of healthy eating, increased healthcare engagement and a strong participant ownership of the garden. There were also other, more unexpected outcomes too. It was noticed that the wellbeing of staff was enhanced, there was an uptake of physical health assessment and those involved in the project developed
horticultural skills.
The project also reignited the lead nurse’s passion for gardening and strengthened leadership and project delivery skills. The project’s greatest success was deep engagement from individuals previously disengaged from healthcare. It’s also a reminder that medication alone cannot solve health challenges.

Tom’s Story
‘Tom’ is a 58-year-old man who has experienced homelessness in the UK for over 20 years. He lives with high blood pressure, alcohol dependence, depression and regularly uses cannabis. Initially referred to a nurse-led clinic due to concerns about his physical health, he was reluctant to engage and often avoided contact altogether.
Tom began to attend the weekly therapeutic gardening sessions. He soon started talking to the nurse about his health and eventually requested a blood pressure check. Over time, he agreed to complete a wellbeing assessment and began taking prescribed medication for his hypertension.
Tom was referred to both addiction and psychological support services, began attending GP appointments and was supported to contact housing services. He reported improved mood, reduced anxiety and a renewed sense of purpose. After nine months of intermittent engagement, his mental health score had improved, reflecting his growing wellbeing and confidence.
Supportive Environment, the Reawakening of Capabilities
Taichung Tzu Chi Nursing Home, Buddhist Tzu Chi Medical Foundation Shu-Ting Chuang.
Florence Nightingale pointed out that a good environment supports health and vitality. In care spaces the environment is more than just a backdrop; it is a vital force in promoting self-realisation for seniors.
The Taichung Tzu Chi Nursing Home has been built around the concept of ‘home’ and a 5H care philosophy: honour, health, heart, happiness and home. Through this H-shaped environmental design and arrangement, even elderly residents with disabilities can enjoy a familiar and safe environment, enjoying the activities they desire—for example, recreating a favourite dish. As the aroma of food permeates the space memories are rekindled, allowing the elderly to connect through warm interactions and rediscover the value of their own abilities.

The Architecture of Healing in Ugandan Hospitals
Sr. Etim Nakewa Sharon, Mbarara University of Science and Technology, Uganda.
In Uganda the concept of healing in hospitals extends beyond medical treatment to include the physical, emotional and cultural well-being of patients. Nurses play a key role in shaping hospital spaces to foster this holistic approach. Their daily interactions with patients give them unique insight into how environments can promote dignity, comfort and recovery.
Many Ugandan hospitals still use historical ward designs, focusing on supervision and efficiency rather than privacy or comfort. Nurses are adapting to these spaces by emphasising patient-centred principles, by advocating for improved ventilation, adequate bed spacing and infection control practices to reduce hospital-acquired infections. These measures protect patients physically and create safer environments that support trust in health care.
Ugandan hospitals often blend resourcefulness with deep community care. While some urban hospitals like Mulago National Referral Hospital in Kampala have modern wards, many rural clinics work with beautiful simplicity – open air verandas for air flow, murals painted by local artists and nurses using natural light and ventilation to keep spaces fresh. Healing here is both medical and social as family members often stay with patients, cooking meals and offering emotional support. This turns hospital corners into lively nests of storytelling and prayer warmth replaces high technology comforts.

Re-envisioning Healthcare Design Using a Planetary Health Lens to Improve the Health and Well-being for All
Trinity Western University, School of Nursing, British Columbia, Canada
Ashley DaCosta, MSN, RN
Barbara J Astle, PhD, RN, FCAN, FAAN
Richard Sawatzky, PhD, RN, FCAN

Architectural render of healing spaces to support well-being and connection (AI visual created by Ashley DaCosta)
In the presented image, picture yourself standing with your feet grounded and connected to the Earth. You take a deep breath of fresh air and see a building that appears welcoming, inviting and representative of the local community; it is a healthcare facility. The building’s façade features animal hieroglyphics that hold significance and reflect species found throughout the community’s lands. Trees and local indigenous plants line the walkways. A garden in bloom borders the entryway with plants that can be harvested and used for cultural ceremonies inside. You walk inside; your eyes are drawn to the inviting wood features and artwork by local artists whom you recognise. You feel a peaceful aesthetic and acknowledge that this healthcare facility has been thoughtfully designed to support well-being and connection.
In the province of British Columbia, Canada, hospital design is being re-envisioned to foster connections with the Earth and all living things. This visionary hospital integrates planetary health which is an emerging field and framework. Planetary health addresses the current environmental crisis through a solutions-oriented, transdisciplinary approach and social movement. It is the understanding that the environment and human health are inseparable. Nurses, trusted advocates of health, social justice and equity, recognise that human health and well-being are deeply connected to the land, climate, air quality, water, food systems and biodiversity. Nurses are uniquely positioned to advance planetary health by influencing the design of healthcare facilities and optimising operational practices to promote health and well-being for all.
Interconnecting this futuristic hospital with nature involves incorporating diversity. This includes integrating different worldviews, knowledge systems and traditions into both the design of the healthcare facility and the practices that take place inside. This shift in healthcare culture challenges the limits of a disease-centric approach by creating spaces that enable traditional medicine, spiritual practices and other cultural traditions. This approach aligns closely with the nursing philosophy of providing holistic care.
Spatial Practice at Changhua Christian Hospital’s Dementia Care Centre, Taiwan
The Modern Practice of the Nightingale Philosophy
Addressing the Dementia Challenge
With the acceleration of global population aging, dementia has become a critical healthcare issue worldwide. As an acquired, comprehensive, cognitive impairment caused by brain pathology, its prevalence rapidly increases with age.
As early as the nineteenth century, Nightingale underscored the deep influence of the healthcare environment. Changhua Christian Hospital (CCH) in Taiwan, adheres to this conviction, regarding the physical space as integral to therapy. We have meticulously designed a space that is not merely a hospital ward but a living space, a resting sanctuary and a secure shelter for patients. We firmly believe that an environment rich in security and nostalgia can help alleviate patient anxiety, stabilise emotions and even contribute to slowing the progression of dementia.
The Core Design of the Reminiscence Ward
In 2015, CCH, with support from the Ministry of Health and Welfare, successfully transformed a 12-bed acute ward into a ‘Reminiscence Ward’, aimed at providing a familiar and therapeutic inpatient environment for dementia patients.
The design planning emphasises three key dimensions:
- Familiarity and memory stimulation
- Safety and sensory guidance
- Fall and wandering prevention
Nurses: Leading the Design from Clinical Insight
The planning of the project was jointly spearheaded by nurses, physicians and designers. By integrating their clinical experience with
environmental design principles, nurses acted as clinical observers, design collaborators and care drivers in the design process. These key roles ensured the space is not only safe and practical but also therapeutic.
Current Status and Future Outlook
The ‘Reminiscence Ward’ design has been used for ten years at CCH. Its features and effectiveness persist, establishing it as a model for dementia care within the hospital. The ward currently houses the ‘Dementia Co-Care Centre,” which integrates medical, nursing, rehabilitation and social work resources, continually advancing a person-centred, therapeutic care environment. CCH’s practice proves that nurses are not just caregivers; they are key decision-makers in healthcare environment design.

Károlyné Boros – University-certified Nurse, MSc, Addiction Consultant, Healthcare Manager
Development of Psychiatric Care with Nursing Participation in Hungary

In 1994 I began working as a nurse in the psychiatric department of a regional hospital in Hungary. From 1995 onward I oversaw daily operations as head nurse.
Early in my career I realised through patient conversations that rehabilitation and social reintegration require more than medication.
I started by improving the physical environment. In collaboration with hospital management, we upgraded bathroom hygiene to facilitate easier cleaning.
In 2012, a European Union grant offered the further opportunity to enhance the environmental conditions for both patients and staff. The project, titled Development of Rehabilitation Services in the Western Transdanubian Region, provided full funding for our department.
We created a separate unit that included a gym, a training kitchen, group rooms, community spaces and a library corner. We renovated the inpatient psychiatric rehabilitation ward and purchased new equipment for psychological assessment, offices and the sports area.
An exhibition of patients’ artworks was created and we invited guest speakers to run thematic programmes.
In 2018 we participated in a five-year project for the first time in Hungary, which renewed the equipment of psychiatric care and the caregiving network. Using European Union funding a Day Therapy Unit was established. This did not require hospital admission so
clients accessed the services as outpatients.
We placed great attention on creating a green environment. Corridors and community spaces were decorated with various plants, nature photographs and paintings.

Thank you to all our sponsors and partners for their contributions to this exhibition.
Nightingale and her Environmental Theory
Much of Nightingale’s ideas were based around nature. She used her publications on nursing to inform readers about the necessities needed in a sick room.
These patients necessities form Nightingale’s Environmental Theory. Her theory is based on the idea the patient should minimise the amount of energy exerted on being stressed trying to manage ascpects of their environment. It is the role of the nurse to ‘fix’ what is out of balance, ensuring tha the room is quiet or thre is enough light for the patient to read or fresh air coming in from a window. For example, a noisy room can be quite distressing for a patient, so rather than the patient trying to seek quiet or exert energy themselves to reduce noise, the nurse should be the one altering or adjusting the environment.
Nightingale had observed in the Crimean War that the wards were dark, cramped, smelly and noisy. While she had tried to relieve this, the building itself had never been intended to be used as a hospital. This made it much more difficult for her to make changes. She could see that introducing natural light and fresh air was beneficial and so following the end of the war, used this experience to think about how a hospital and other spaces used for healthcare could be best designed to maximise the connection with nature and ensure that the right balance was created.
Nightingale was a prolific writer throughout her life, including a number of published texts written from the 1850s onwards. Among these are two of her most famous works, ‘Notes on Hospitals’ and ‘Notes on Nursing: What It Is and What It Is Not’. These two important texts, written in the years following the Crimean War, outline all of Nightingale’s thoughts about the best environment for patients to heal.

Notes on Hospitals
First published in 1859, Notes on Hospitals was a publication of two papers that Nightingale wrote to be presented at the National Association for the Promotion of Social Science in Liverpool, October 1858. The report includes much of the evidence that she
put forward to the Royal Commission on the state of the Army that she had presented the year before. Throughout the book,
Nightingale gives evidence in the form of tables and large amounts of data.
Pavilion Hospitals and Nightingale Wards
Following the publication of her books, Nightingale became known across the world as an authority on the design of hospitals and she was soon corresponding with various architects and hospital governors globally.
Nightingale felt that new hospitals should be designed to the pavilion style as this best aligned with her Environmental Theory. She did not invent this idea as hospitals in Europe had started to use this type of design earlier in the century but she eagerly adopted the principles for recommendation.
The pavilion design was based around a series of individual buildings that were connected by a singular walkway or corridor. Each building would have its own facilities, ensuring they were self-contained to minimise cross contamination. As each part of the hospital was its own separate building, the rooms could be designed to have windows on either side ensuring light and air circulates to all parts of the room, particularly if built on a North/South axis.
The individual wards in a pavilion style hospital were large oblong shaped rooms with windows on either side and two lines of beds underneath the windows. In the centre of the room would be heaters or desks and tables.
These types of wards would soon become known as ‘Nightingale Wards’, and alongside the healthy environment created for patients, these wards were designed in a way that streamlines work for the nurses working on the ward.

St Thomas’ Hospital, London
St Thomas’ Hospital has existed in London for hundreds of years and while the foundation date for the hospital is not known, it was renamed in the 12th century for St Thomas Becket and it is suggested that it was quite an old hospital at that time. The first site was by London Bridge, near to the location of Guy’s Hospital. By the 1860s, the hospital needed to move as the government served a compulsory purchase notice on the site to build a railway viaduct.
While existing on several temporary sites across the 1860s, the hospital found its new home on the banks of the River Thames, on the newly constructed Albert Embankment. The architect Henry Currey was appointed to design the hospital.
Despite Nightingale’s horror at the idea of a hospital so close to a river, she was still able to have some influence on the design, and the pavilion style was chosen. The hospital was built with six pavilions, connected with a corridor and administrative block at the centre. Between the pavilions were gardens that could be used by staff and patients and many of the wards had balconies that allowed patients outside to overlook the Thames and the Houses of Parliament.
Seventy years after the opening of the hospital, the northern part of the hospital was severely damaged by air raids during the Second World War and extensive rebuilding of the hospital took place over the following decades. While not all the pavilions remained standing, the surviving pavilions are still in use today. These can be best viewed from Westminster Bridge.

The exhibition is now on at the Florence Nightingale Museum until December 2026.
Exhibition is included with general admission.
